In the complex world of female infertility, laparoscopy stands as a ray of hope. It holds the key to diagnosing and addressing conditions like endometriosis, pelvic adhesions, fibroids, and ovarian cysts, often silent culprits hindering conception. Laparoscopy procedure not only diagnoses but offers a therapeutic pathway, delicately navigating reproductive complexities. This exploration unveils the pivotal role of laparoscopy in reshaping fertility treatment, illuminating aspiration for individuals and couples navigating the intricate landscape of infertility.
In this Article
Understanding Female Infertility
Female infertility is a complex puzzle, with each piece adding to the intricate web of challenges in the journey toward conception. Exploring deeper, we uncover common factors such as endometriosis, pelvic adhesions, fibroids, and ovarian cysts—silent adversaries that silently obstruct the path to conception.
Endometriosis
Endometriosis, a stealthy condition where tissue similar to the lining of the uterus grows outside it, often goes undetected. Laparoscopy becomes a key player in diagnosing and treating this elusive culprit. By removing abnormal growths, laparoscopy uses aims to restore reproductive potential.
Pelvic Adhesions
Pelvic adhesions, bands of scar tissue that form between pelvic organs, can severely limit fertility. Laparoscopy’s minimally invasive approach delicately addresses adhesions, liberating fertility prospects without the invasive impact of traditional surgery.
Fibroids
Fibroids, noncancerous growths in the uterus, can pose significant hurdles to conception. Laparoscopy offers a means to manage and remove fibroids, paving the way for couples to regain their foothold towards parenthood.
Ovarian Cysts
Ovarian cysts, fluid-filled sacs on or within the ovaries, can disrupt the delicate balance of fertility. Laparoscopy, by delicately addressing and removing cysts, becomes a valuable tool in clearing the path to conception.
The Laparoscopy Procedure
The procedure of laparoscopy encompasses meticulous stages, starting from comprehensive pre-operative preparations, progressing through the surgical process, and culminating in post-operative care and recovery:
Pre-operative Preparations
Before commencing the laparoscopic journey, a thorough preparation phase is initiated. Patients undergo a series of assessments to ensure their physical and emotional readiness for the procedure. Clear and open communication between patients and healthcare providers is paramount during this phase, fostering trust and mutual understanding.
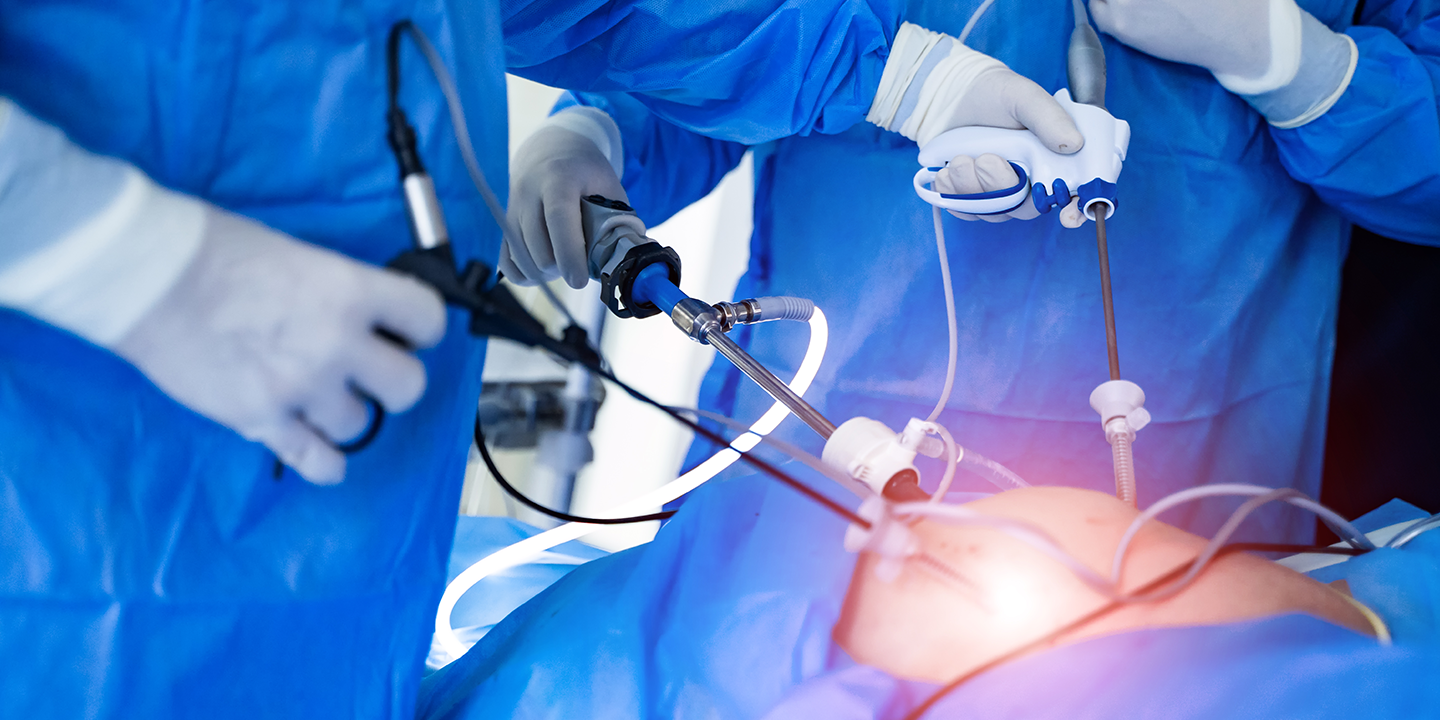
The Surgical Process
Laparoscopy unfolds as a coordinated orchestration between the surgeon and sophisticated technology. Utilizing small incisions, miniature cameras, and specialized instruments, this approach adeptly addresses identified concerns. Its distinguishing feature lies in its capacity to significantly reduce scarring, alleviate pain, and expedite overall recovery when juxtaposed with traditional surgical methods.
Post-operative Care and Recovery
Following the surgery, a meticulous plan for laparoscopy for infertility recovery time is implemented. Patients are carefully guided through the healing process, emphasizing a swift return to normal activities. The notably reduced recovery duration associated with laparoscopy underscores its patient-centric approach, prioritizing optimal recuperation.
Moreover, understanding the aspects of laparoscopy for infertility cost is integral for individuals considering this procedure as a part of their fertility treatment plan. However, it’s important to note that discussing specific costs should be done directly with healthcare providers to ensure clarity and comprehensive information.
Role of Laparoscopy in Treating Female Infertility
When it comes to combating female infertility, laparoscopy offers targeted solutions to a spectrum of underlying issues. Let’s delve into the specific roles this procedure plays in addressing various fertility challenges:
Addressing Endometriosis
Endometriosis, often an unseen adversary, silently chips away at a woman’s fertility. Laparoscopy steps in as a diagnostic and therapeutic tool, allowing the laparoscopy surgeon to visualize and remove endometrial tissue outside the uterus. By excising these growths, laparoscopy not only alleviates pain but also enhances the chances of conception. The restoration of a conducive environment for pregnancy becomes plausible post-surgery.
Dealing with Adhesions
Pelvic adhesions, a consequence of surgeries, infections, or inflammation, create a web of obstacles within the reproductive system. Laparoscopy enables surgeons to delicately dissect these adhesions, freeing organs and restoring their functionality. By untangling these barriers, laparoscopy revives the possibility of natural conception or aids in the success of assisted reproductive techniques.
Managing Fibroids
Fibroids, benign tumors in the uterus, can significantly impair fertility. Laparoscopy offers a strategic approach, allowing for the removal of problematic fibroids while preserving the uterus. This targeted removal minimizes the impact on fertility, often resulting in improved reproductive outcomes. With the removal of these growths, the path to conception becomes less obstructed.
Tackling Ovarian Cysts
Ovarian cysts, though common, can impede fertility by affecting ovulation or causing disruptions in the reproductive cycle. Laparoscopy provides a means to address these cysts, either by excision or drainage, restoring normal ovarian function. By resolving these cysts, the hurdles hindering conception are diminished, potentially enhancing the chances of successful pregnancy.
Benefits and Risks
The landscape of laparoscopy procedure in treating infertility is marked by both benefits and risks. Understanding these elements is crucial for informed decision-making.
Benefits of Laparoscopy in Treating Infertility
Minimal Invasiveness: Reducing Surgical Impact
- Smaller incisions translate to less scarring and reduced post-operative pain.
- Quicker return to normal activities, fostering a faster recovery.
Faster Recovery: Enabling Quicker Return to Fertility Treatments
- Reduced recovery time allows couples to resume fertility treatments sooner.
- Enhanced patient satisfaction and improved overall well-being.
Enhanced Precision: Targeted Treatment Approach
- Laparoscopy’s precision minimizes damage to surrounding tissues.
- Greater accuracy in identifying and addressing fertility-related issues.
Potential Risks and Complications
Surgical Risks: Weighing the Possibilities
- Infection, bleeding, or damage to surrounding organs are potential surgical risks.
- Though rare, these risks necessitate thorough consideration and discussion with healthcare providers.
Post-operative Concerns: Navigating Recovery Challenges
- Pain and discomfort during the recovery phase are common but manageable.
- Open communication with healthcare providers is key to addressing and alleviating concerns.
The Road Ahead
As we look to the future, the prospects of laparoscopy in infertility treatment appear promising. Ongoing advancements and research continue to refine and expand the scope of this laparoscopy for infertility procedure, offering hope to those navigating the intricate landscape of fertility challenges.
Final Thoughts
Overall, laparoscopy stands as a transformative force in female infertility treatment. Its targeted approach in addressing endometriosis, adhesions, fibroids, and cysts redefines the road to conception. As we envision a brighter fertility landscape, the role of laparoscopy remains paramount. The promise of laparoscopy endures, illuminating a pathway filled with possibilities for those seeking to overcome the challenges of infertility.
Why Choose Queen’s Gynecology?
At Queen’s Gynecology, expertise converges with compassionate care in our approach to laparoscopy for treating infertility. Our renowned fertility specialists leverage cutting-edge techniques, offering precision and minimal invasiveness in addressing reproductive challenges. With a patient-centric focus, we guide individuals through their fertility journey, ensuring comprehensive support and tailored treatment plans. Our commitment to excellence and a track record of successful outcomes solidifies Queen’s Gynaecology as a premier destination for navigating infertility with trust and expertise.