About 10 to 12 percent of women develop a hormonal disorder called PCOS. Women with PCOS are also noticed to have insulin resistance, which leads to too much insulin in the body, which can increase the risk for type 2 diabetes. If you have been diagnosed with PCOS, your gynecologist will work with you on the right treatment plan. Also, they will help you to understand more about PCOS and insulin resistance and how to manage it well for a healthy lifestyle. If you seek an expert gynecologist in Delhi, visit Queen’s Gynecology to get yourself checked and treated. The clinic also has dieticians as a part of the medical team treating this disorder to assist with things you can control, including focusing on the following areas and helping you to focus on vital areas.
In this Article
- 1 What Is PCOS and Insulin Resistance?
- 2 The Impact of Diet and Lifestyle on Insulin Resistance
- 3 Medical Approaches to Managing Insulin Resistance in PCOS
- 4 Preventing Complications: Treating Insulin Resistance Early
- 5 Balancing Hormones and Insulin for PCOS Management
- 6 Your Roadmap to a Healthier Life with PCOS and Insulin Management
- 7 FAQ’s
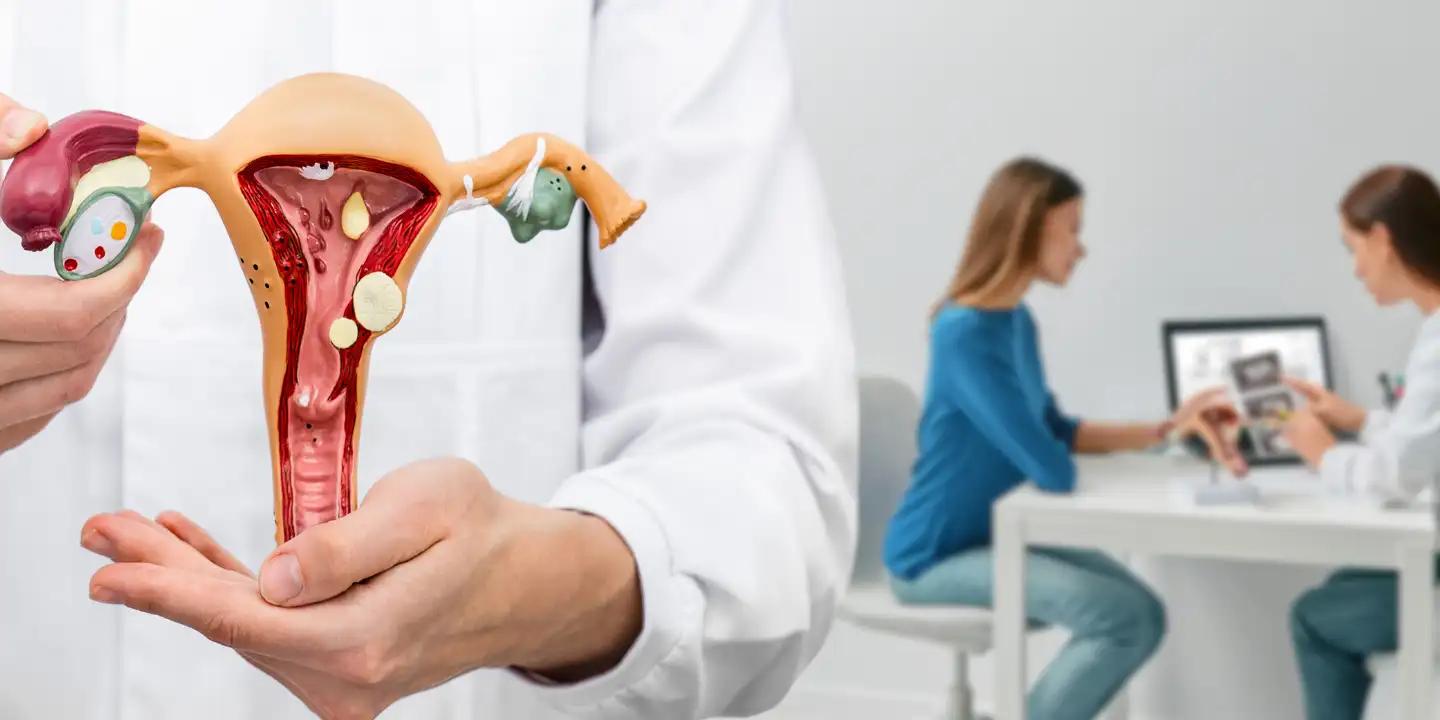
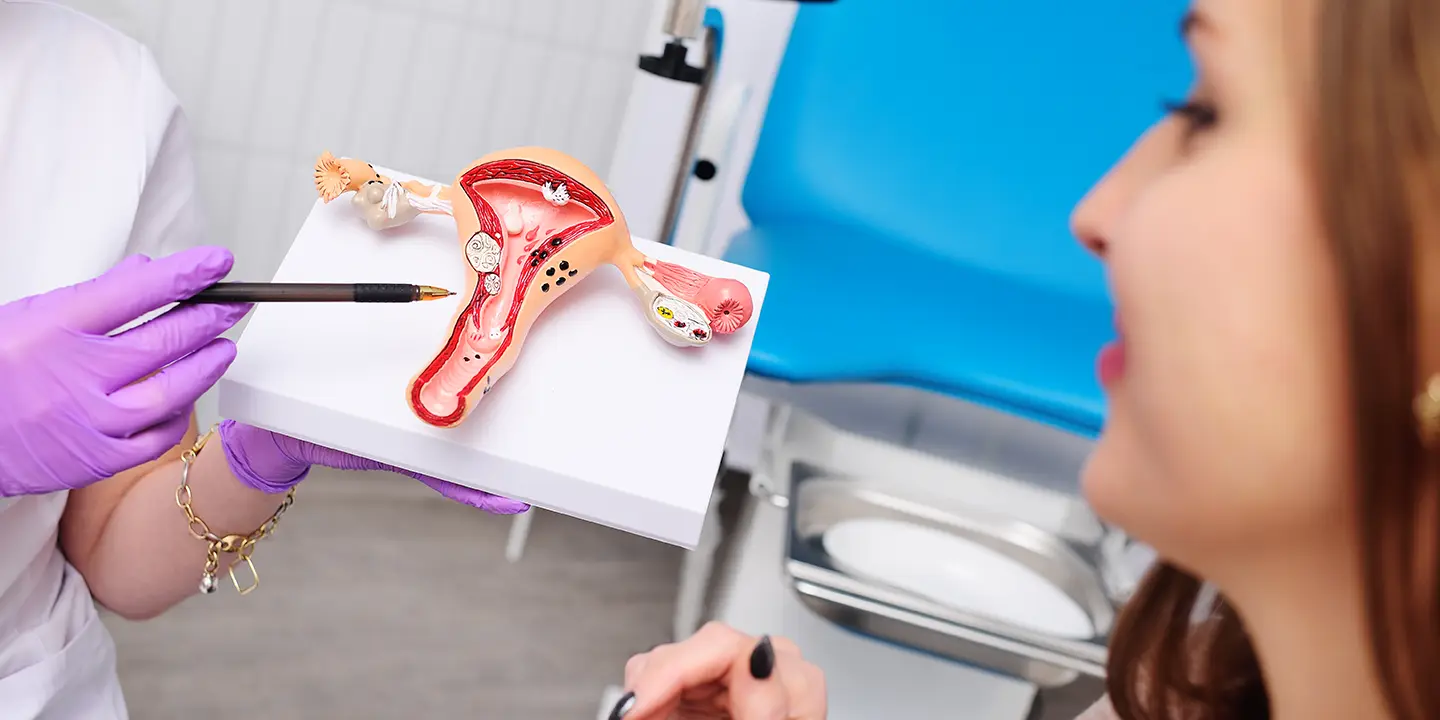
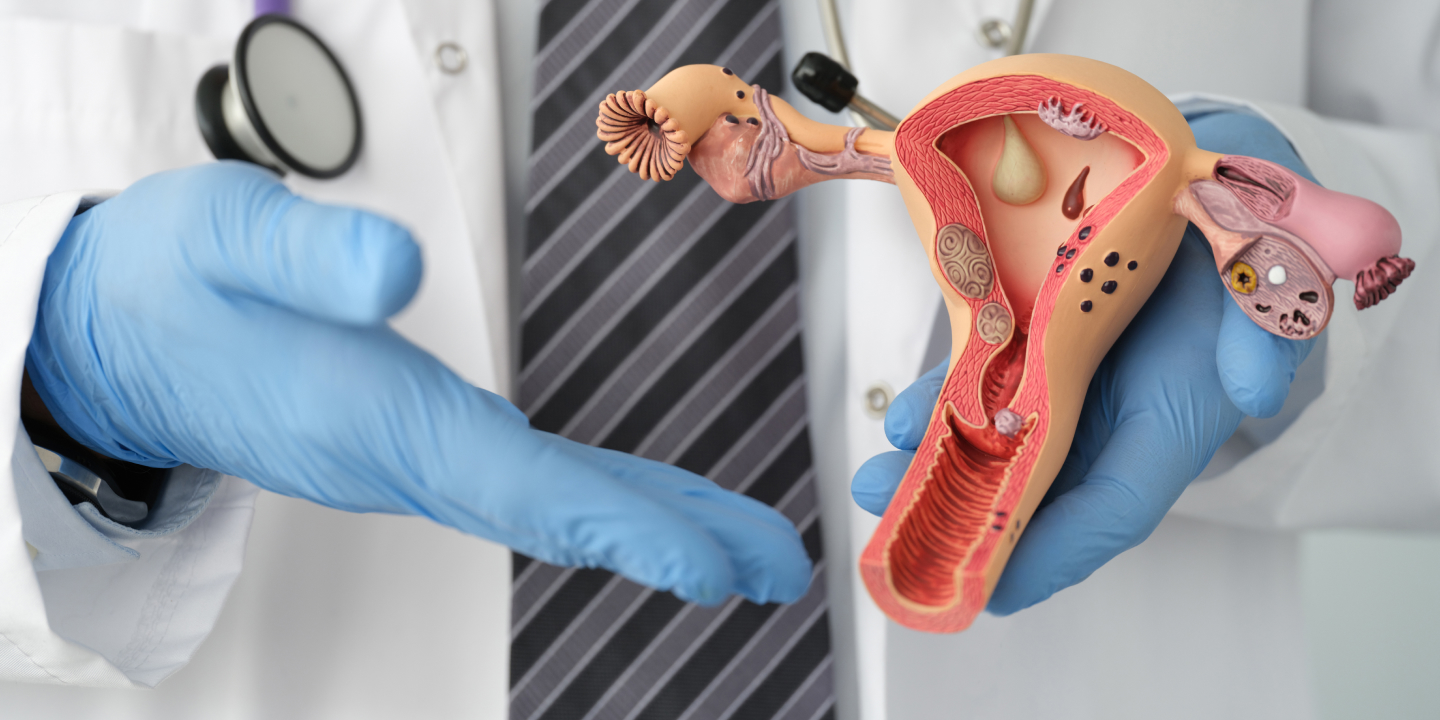
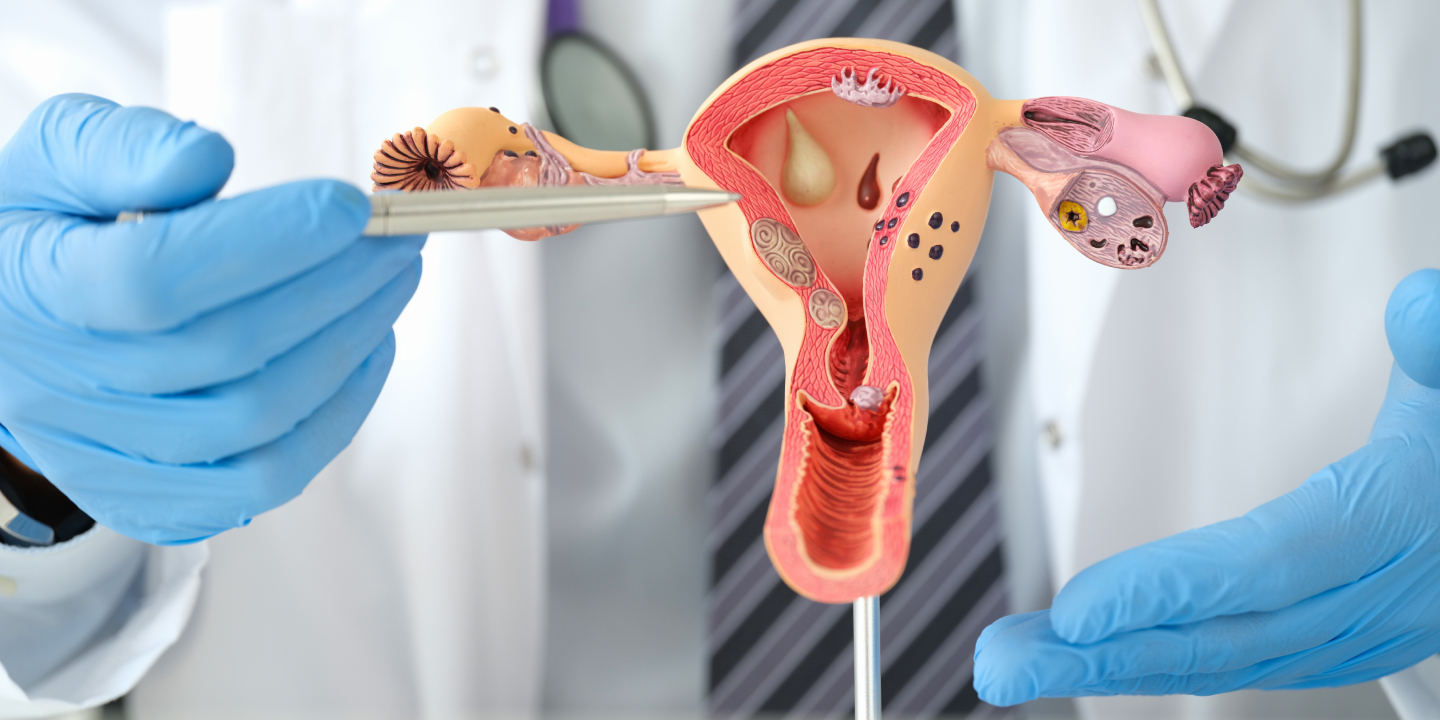
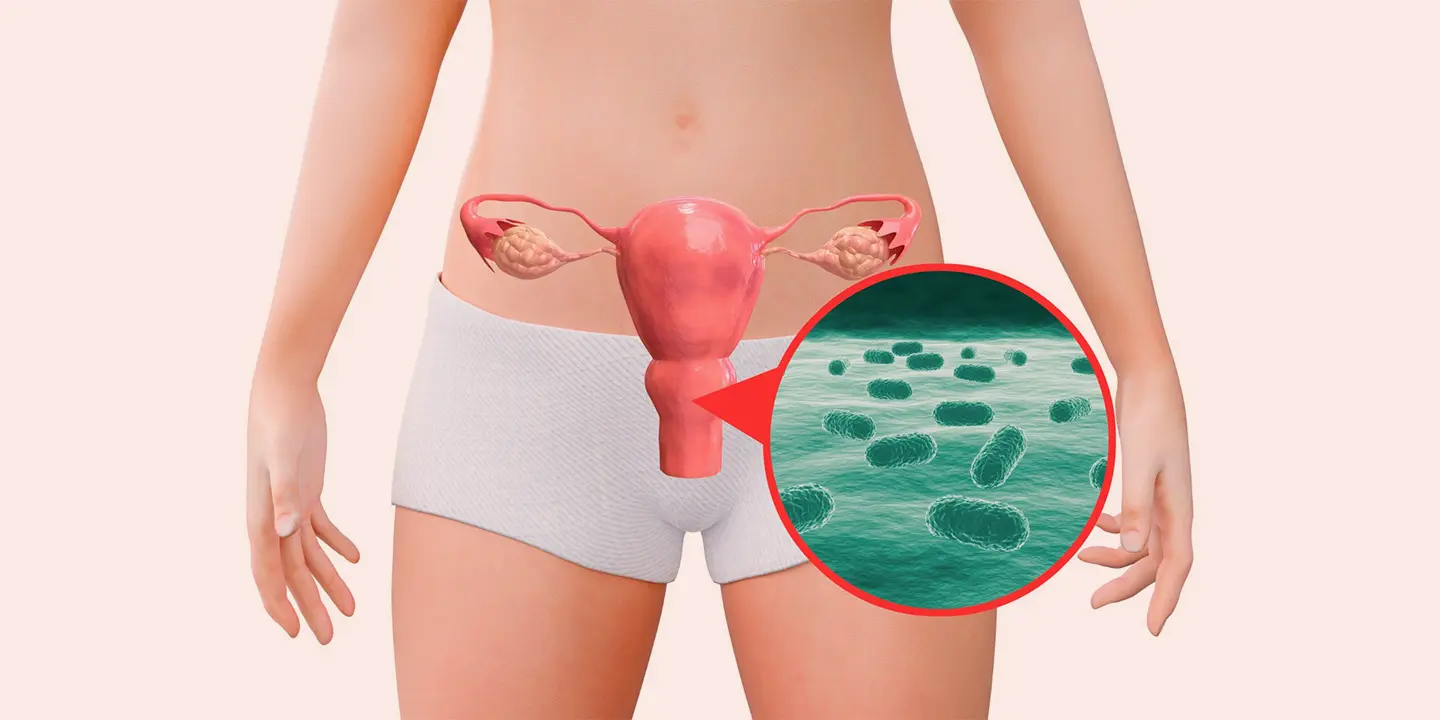
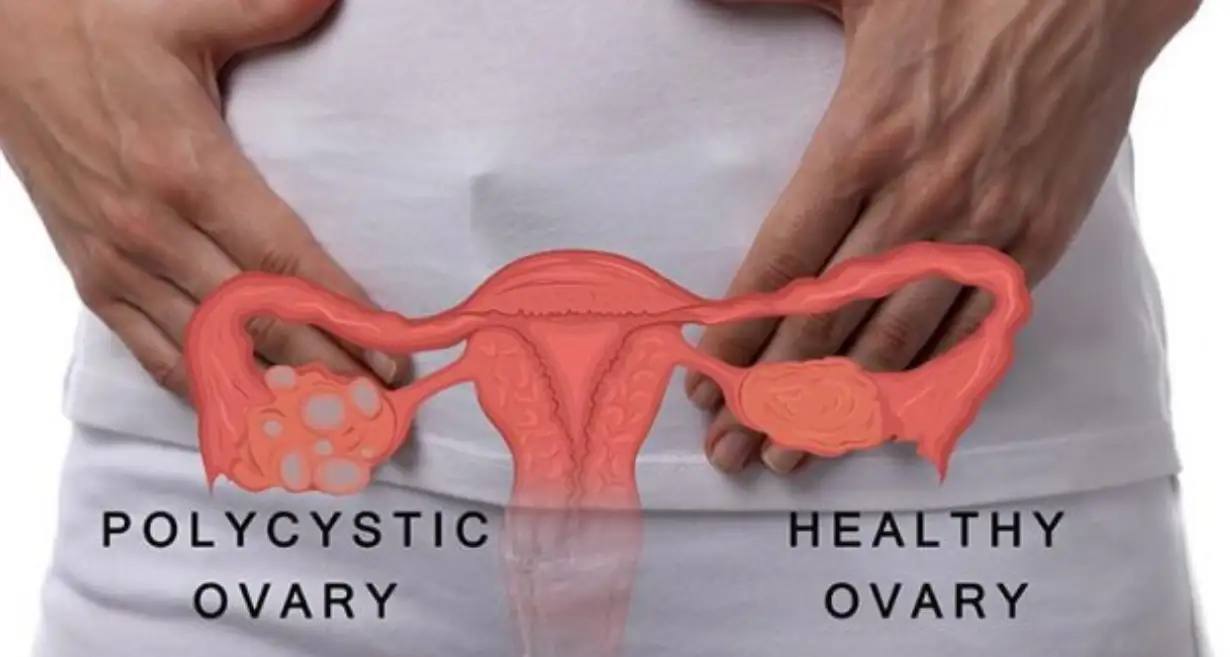
What Is PCOS and Insulin Resistance?
Polycystic ovary syndrome PCOS is a health issue that affects about 6 to 10 percent of women, and women with this condition have hormonal imbalances and metabolism problems that may affect their overall health. The leading cause of PCOS is an imbalance of reproductive hormones, as these hormones create issues in the ovaries. In the ovaries of women with PCOS, the egg may not develop as it should, or it may not be released during ovulation as it should usually.
Insulin resistance is a complex condition that increases a person’s risk of developing diabetes, and you can be insulin-resistant for many years without knowing it. It is a condition linked to prediabetes in which your body is unable to respond to the amount of hormone insulin it is producing. Your pancreas makes insulin and helps protect your body from getting too much sugar ( glucose) as too much of it is harmful to your health. As long as the pancreas can make enough insulin to overcome your cell’s weak response to insulin, your blood sugar levels will stay in a healthy range. When your cells become too resistant to insulin, it leads to high glucose levels. You cannot prevent or avoid risk factors of developing insulin resistance. It can take steps to reduce them by losing weight. Insulin resistance is considered one of the key physiological imbalances in almost all cases of PCOS and is also a symptom of PCOS. Testing for insulin resistance can help you to rule out other conditions as well that are commonly misdiagnosed, like PCOS.
Related Blog: PCOS Diet Guide: What to Eat and Avoid
The Role of Insulin in the Body
Insulin is produced by the pancreas, a gland located in the abdomen, and which is this hormone’s one of the primary role to controlling blood sugar levels to prevent many issues. A healthy body produces insulin precisely, which allows the body’s metabolism to be balanced. Insulin helps shuttle blood sugar to your muscles and fat as liver cells and glucose enter the body from the foods you eat. The time insulin moves into your cells, your blood sugar returns to normal. Insulin plays a vital role in the body as
- It modifies the activity of specific enzymes that impact protein synthesis and also builds muscles following sickness or injury.
- Insulin also helps in making healthy changes in fat cells and is vital to the absorption of amino acids and potassium.
- The hormone also manages the excretion of sodium in the urine and also enhances memory and learning capabilities.
How PCOS and Insulin Resistance Are Connected?
PCOS is an endocrine condition closely connected to insulin resistance, however, not all with PCOS have insulin resistance. Also, insulin resistance is not a part of the formal diagnostic criteria for PCOS as well. But PCOS, as well as insulin levels and the body’s ability to use insulin, are connected to each other. High insulin is not only a symptom of PCOS. Still, it is also a significant driver of the condition, as it can impair the population and cause ovaries to produce excess testosterone. Increased insulin levels contribute to inflammation and other metabolic complications like PCOS. However, the connection is not exactly clear because insulin resistance does not affect everyone in the same way. Some may develop PCOS, and some may not. Both insulin resistance and PCOS contribute to infertility because of the hormonal changes linked with the two.
Symptoms and Signs of Insulin Resistance in PCOS
Though a woman can have insulin resistance and not have any symptoms, there are some warning signs of insulin resistance in PCOS that you must notice:
- Dark pigmentation on the side of the neck, armpits area, and groin and thickening of the skin
- High insulin level that leads to increased hunger
- Weight gain and difficulty losing it
- Craving for sweet, salty foods and carbs
- Frequent urge for urination
- Increased hunger and thirst
- Tingling sensation in feet and hands
It is best to consult your gynecologist for further procedures when you experience PCOS insulin resistance symptoms.
The Impact of Diet and Lifestyle on Insulin Resistance
Certain diets, as well as lifestyle habits, can affect the risks related to insulin resistance. In fact, eating or avoiding certain foods can help improve insulin sensitivity, reduce insulin resistance, and decrease a person’s risk of developing type 2 diabetes. Eating foods with a low to medium glycemic index and limiting foods with a high glycemic index can help you reverse and manage insulin resistance effectively. It is vital for you to know about heart-healthy fats, proteins, and the appropriate quantity and quality of carbs that are crucial to determine a diet for patients with PCOS insulin resistance. Pairing the listed nutrients in the correct portion is the key to a perfect diet.
Related Blog: Irregular Periods Management in Women Suffering From PCOS
Medical Approaches to Managing Insulin Resistance in PCOS
Not only diet and lifestyle but there are ways to manage insulin resistance in PCOS medically. Metformin is a prescription medication prescribed by a doctor as it works by reducing the production of glucose in the liver, a problem for women with PCOS. It helps to decrease insulin resistance and effectively manage PCOS symptoms. Although metformin also plays a vital role in reducing insulin resistance, it does not normalize insulin resistance in PCOS and can have side effects that may limit compliance. Speaking to your doctor before managing your PCOS with metformin is necessary as it should be taken under the guidance of experts. At Queen’s Gynecology, expert doctors may prescribe medication to regulate menstrual cycles and encourage ovulation. The condition cannot be cured well, but PCOS treatment can be done by managing its symptoms well.
Preventing Complications: Treating Insulin Resistance Early
When a person has insulin resistance, their pancreas makes extra insulin to make up for it. For some time, this can work, and your blood sugar levels will stay normal. But with time, the pancreas could not effectively keep up. Thus, it is vital to treat insulin resistance early because if you don’t make changes in the way you eat and exercise, your blood sugar levels will rise until you have prediabetes, which can worsen your other linked conditions like PCOS. There are effective ways to combat insulin resistance at early stages. You can do this by losing weight, exercising more, or taking a prescribed insulin-sensitizing medication. All these can help you get back to good blood glucose control and better health.
Balancing Hormones and Insulin for PCOS Management
PCOS is abnormally caused by hormonal imbalance, and it increases a woman’s risk of developing type 2 diabetes, infertility, and uterine cancer. Hormone balancing and insulin levels management can help manage symptoms of PCOS and improve overall health; thus, it is best to make conscious steps towards better habits and lifestyles. You can effectively maintain your hormonal imbalance and insulin levels by:
- Maintaining a healthy diet plan
A balanced diet will help you to regulate insulin levels and improve hormone regulation. PCOS is a condition that requires management of both, and women must try to consume a diet that is low in processed foods and added sugars. Also, focus on consuming plenty of fruits, veggies, lean protein as well as healthy fats.
- Maintain a healthy weight
It is another way to achieve a healthy weight and to improve hormone regulations. Losing excess weight will assist in regulating insulin levels, improve menstrual cycles, and reduce PCOS symptoms.
- Exercising regularly
By regular exercise routines, toys can effectively regulate hormones and improve insulin resistance. It helps to treat and prevent obesity, which is a common symptom of PCOS. You make a routine to walk daily for at least 30 minutes.
- Manage stress
Managing stress also helps you to manage hormone imbalance and insulin levels as it contributes to them. You can indulge in yoga, meditation, and deep breathing exercises.
Related Blog: Treatment of Acne Caused Due to PCOS Problems Effectively
Your Roadmap to a Healthier Life with PCOS and Insulin Management
Your roadmap to a healthier life with PCOS and insulin management will start by consulting the gynecologist who will help you with PCOS. Visiting the best gynecologist will help you to develop a comprehensive treatment plan as per your needs. Visit Queen’sGynecologyy, one of the best clinics in Delhi for the treatment of PCOS, as it offers a team of experts that’s courses of gynecologists, PCOS experts, surgeons, reproductive and infertility specialists, nutritionists, and diabetes experts for insulin resistance. The clinic has the best PCOS treatment plans to correct menstrual irregularities and many other PCOS symptoms.
Related Blog: PCOS and Weight Gain
Conclusion
PCOS can be difficult to manage, but hormone regulation can support and assist in improving its symptoms and overall health. There are several treatment avenues available to help alleviate not only the underlying cause of PCOS but also many of its symptoms. It is best to consult an expert PCOS specialist to get yourself checked and treated. If left untreated, Polycystic Ovary Syndrome can offer many severe complications as well as health risks. Visit Queen’s Gynecology to get expert advice and a PCOS treatment plan as soon as possible. Early diagnosis, lifestyle changes, and proper medical guidance can assist in reducing the risks and effectively managing PCOS-related complications.
FAQ’s
A healthy lifestyle is the best and most effective way to manage PCOS symptoms effectively and permanently. You can do it by consuming a healthy, balanced diet, doing regular physical activity, maintaining a healthy weight, and reducing or avoiding smoking and excessive drinking.
Living with PCOS can be extremely daunting, but the first thing that you can do to cope with it is to learn to relax and let go of things that can add to your stress. Make sleep your priority, say no to stress, eat well, and always get your body moving. All of these can help you to manage PCOS well. Also, get in touch with PCOS specialists to know all about PCOS treatment plans and get some lifestyle tips.