Around 1-17% of women globally suffer from Vaginismus, a condition that leads to painful sexual intercourse due to an involuntary tensing of the vagina. Not just during sexual intercourse, women suffering from vaginismus also experience pain during the insertion of a tampon or a physical examination.
Most women experiencing vaginismus report feeling pain during penetration and have no issues with sexual arousal. Although the condition isn’t due to any prevalent physical abnormalities, there could be multiple reasons why women experience vaginismus.
This article will explore more about the basics of vaginismus, its potential causes, and how you can treat the condition.
In this Article
Who Are More Prone to Developing Vaginismus?
Despite so many women suffering from it, it is still difficult to pinpoint how common vaginismus is exactly. It is commonly noted that most women in their late teens and early adult age experience the symptoms, especially when engaging in sexual intercourse for the first time.
Some women experience the symptoms later in life, leading to involuntary spasms and contractions during any form of vaginal penetration.
One of the biggest issues with vaginismus is the stigma surrounding it. Most women are often too embarrassed to even talk about the condition, and instead, prefer being in pain or avoiding sexual intimacy.
What are the Causes of Vaginismus?
Although Vaginismus doesn’t have a particular cause, healthcare providers and researchers believe that untreated vaginismus can often lead to a variety of physical or sexual issues.
The classification of pain can be classified into three types:
Entry pain – Caused due to poor lubrication, injury, trauma, irritation, inflammation, skin disorder, vaginal agenesis, etc.
Deep pain – Caused by a series of illnesses, surgical complications, or medical treatments.
Emotional factors – Caused by psychological issues, stress, and a history of sexual abuse.
Some of the common potentials causes behind vaginismus or painful intercourse include:
- Experiencing vaginal tears after childbirth
- Anxiety disorders
- Post-surgical complications from a previous surgery
- Unexplored negative feelings about sexual intercourse
Note: If you have vaginismus, conditions like an active urinary tract infection (UTI) or yeast infection can make the situation worse.
What are the Symptoms of Vaginismus?
With the potential causes of vaginismus out of the way, let us shift our focus to the symptoms. Paying attention to the vaginismus symptoms can help you get a quicker and more holistic diagnosis.
Since the condition of vaginismus is quite taboo, it isn’t surprising that most women often brush the symptoms under the rug. At Queen’s Gynecology, we urge you to prioritize and pay close attention to your symptoms.
The quicker you identify and acknowledge your symptoms, the easier it becomes for you to get the relevant treatment you need to overcome the complications.
The following are the most common symptoms:
- Feeling discomfort or excruciating pain during sexual intercourse
- Experiencing muscular spasms and pain during pelvic exams or when inserting a tampon
- Experiencing deep pain with a thrusting motion
- Burning pain even hours after sexual intercourse
- Throbbing pain that lasts for hours
If you experience recurrent pain during any form of penetration in your vagina, it is a matter of serious concern that needs immediate medical consultation. Don’t brush aside these symptoms. Prioritize them instead. Consulting a doctor at the right time can not just help you navigate through these symptoms but also boost your self-image.
How is Vaginismus Diagnosed?
At Queen’s Gynecology, we prioritize providing our patients with a safe space to discuss their symptoms and their concerns without any judgment. Given that most women are often embarrassed to talk about the symptoms, it isn’t surprising that we encourage open discussions.
If you are experiencing any offbeat symptoms, the diagnosis starts with getting answers to the following questions:
- When did you first notice the symptoms and the allied complications?
- How often do the pain and discomfort happen?
- What kinds of events trigger the pain and the discomfort?
We also discuss the patient’s sexual history and that might involve dipping the toes into a few sensitive subjects as well. Depending on the answers to these above questions and the symptoms described by the patient, we advise a pelvic exam to confirm the suspicions.
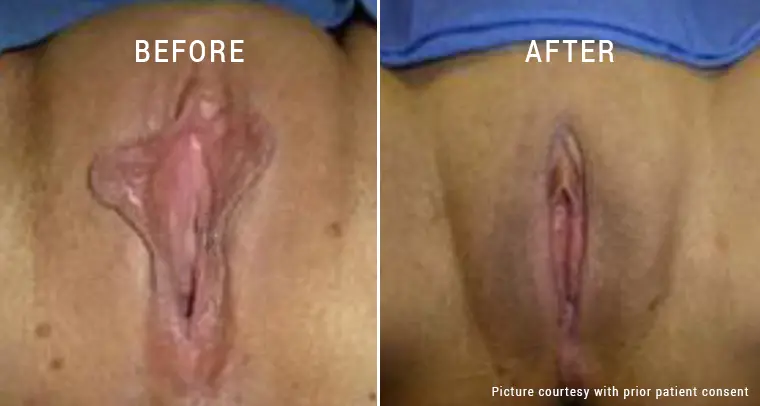
A pelvic examination helps in ascertaining whether or not the patient actually has vaginismus or any other underlying complication like vaginal atrophy or vulvar vestibulitis.
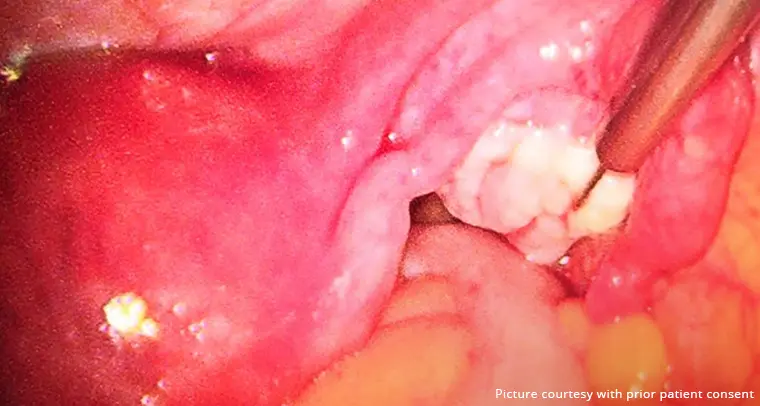
During the examination, we look for signs of involuntary contraction or muscular spasms. Besides that, we also look for signs of scarring or infection in the vagina to determine other complications that could be contributing to the pain.
If there aren’t any visible physical “signs” that could contribute to the involuntary spasms or contractions, it confirms that the patient has vaginismus.
What are the Common Treatment Methods for Vaginismus?
Vaginismus treatment typically starts with medications and can later expand with other forms of therapy to further regulate and reduce the pain and discomfort in the vagina.
At Queen’s Gynecology, we follow a multidisciplinary approach to treating vaginismus. Kindly remember that vaginismus can’t be solely treated with psychological counseling. You need tailored treatment to not just reduce the pain but also to overcome the fear that’s associated with sexual intercourse due to this condition.
Some of the most effective treatment options include:
Medications
One of the most common reasons for experiencing pain during intercourse is poor lubrication. Depending on your medical history, if you are on any kind of medicine that’s contributing to lubrication problems, we focus on replacing those medications first.
Additionally, the drug ospemifene is also FDA-approved and effective in treating mild symptoms of vaginismus in women. It also improves lubrication in the vagina.
Vaginal dilatory therapy
These are tube-shaped devices that are inserted into the vagina to stretch the vagina and reduce the pain and discomfort and reduce sensitivity in the vagina as well.
In some cases where our patients report experiencing excruciating pain, we also prescribe topical therapy like lidocaine to reduce and relieve the pain that comes with vaginismus or during any form of penetration.
Pelvic floor physical therapy
Another lifestyle and physical change that has promising benefits in elevating pain is a physical therapy which improves the flexibility of the vaginal and pelvic floor muscles. These exercises also train the patient to relax their pelvic floor muscles to eventually find the ultimate comfort instead of experiencing excruciating pain.
Does Botox Help with Vaginismus?
Botox is a popular neuromodulator that helps with muscle relaxation when injected. Since vaginismus leads to involuntary muscle spasms and contraction in the vagina, injecting the vaginal muscles with botox alleviates the symptoms to an extent.
Women who have affected sexual life due to vaginismus often get botox injections to reduce the involuntary contractions in the vagina. In patients with vaginismus, the botox is directly injected into the bulbospongiosus muscle, which is found around the opening of the vagina.
The effects of one botox injection last for 3-5 months, following which the same has to be reapplied.
Conclusion
Women suffering from vaginismus often experience issues related to their sexual life. If you are experiencing any of the mentioned symptoms and don’t want the condition to take a toll on your quality of life, getting medical help is crucial. It can be treated and you can experience a normal sex life. Therefore, it is important to seek help at the right time.
At Queen’s Gynecology, we are here to provide patients with a safe and non-judgmental space to discuss the symptoms and then follow a line of treatment to elevate the physical, sexual and emotional well-being of the patient.
For more details, contact us at https://queensgynecology.in/contact-us.
FAQs
Vaginismus is an involuntary condition, which means that no one has control over the condition. Since the exact cause behind the condition isn’t known, there are no proven ways to prevent vaginismus.
Most women with vaginismus don’t experience any prevalent symptoms after getting proper treatment. However, successful treatment takes some time, so ensure that you are patient throughout the process.