Calcified fibroids are a relatively common gynecological condition that affects many women worldwide.
These non-cancerous growths, also known as uterine fibroids, undergo a unique process of calcification, leading to potential complications and discomfort.
In this post, we analyze the key elements of calcified fibroids, including their distinct symptoms, underlying causes, and available treatment options. And if you’re seeking best fibroids treatment in Delhi, visit Queen’s Gynecology right away.
Understanding these crucial factors can empower women with the knowledge needed to make informed decisions about their health and seek appropriate medical care.
In this Article
What Are Calcified Fibroids?
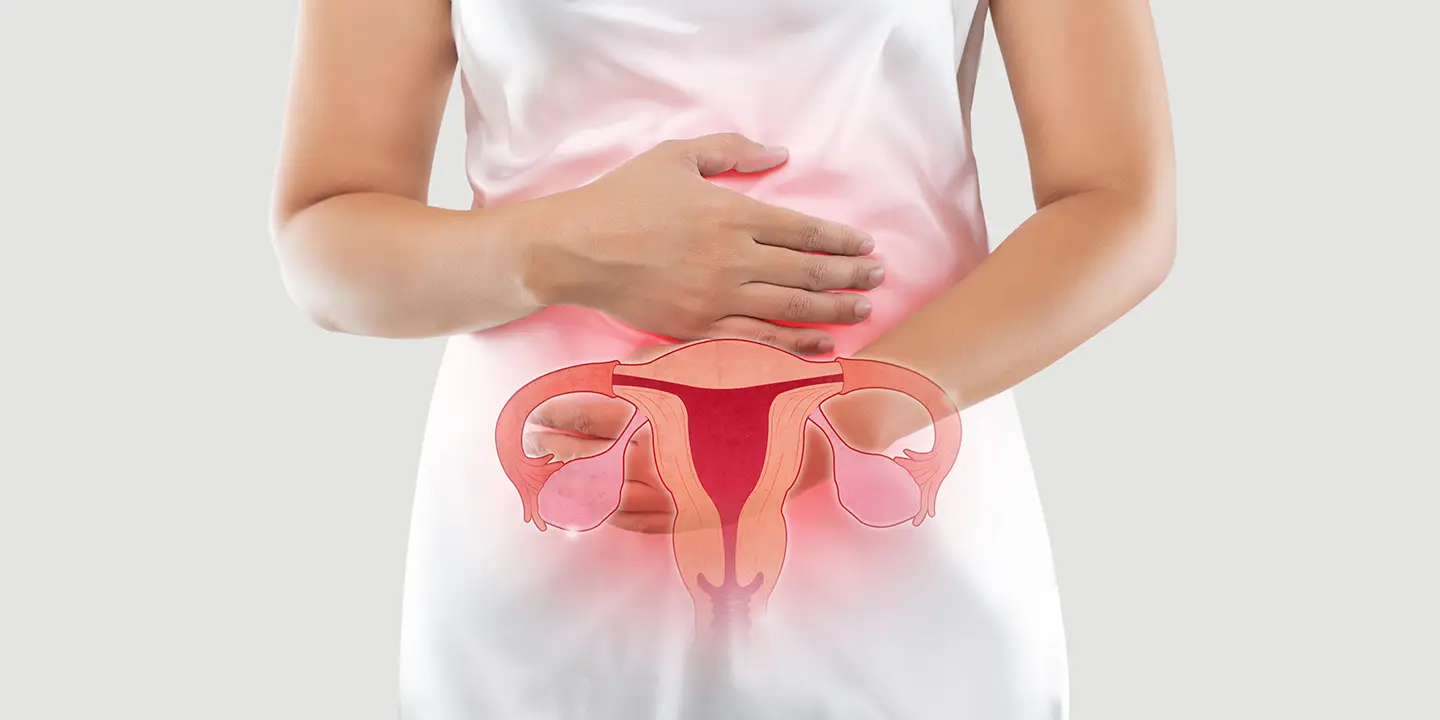
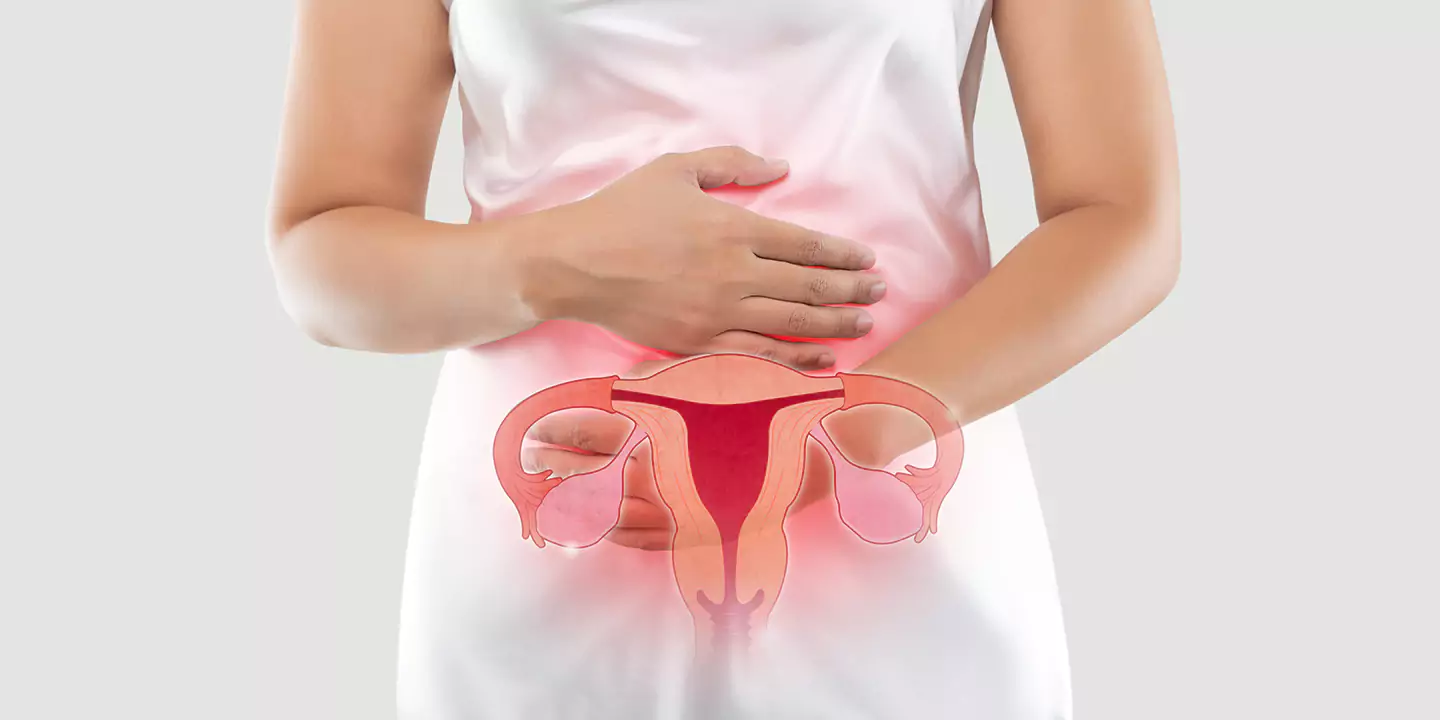
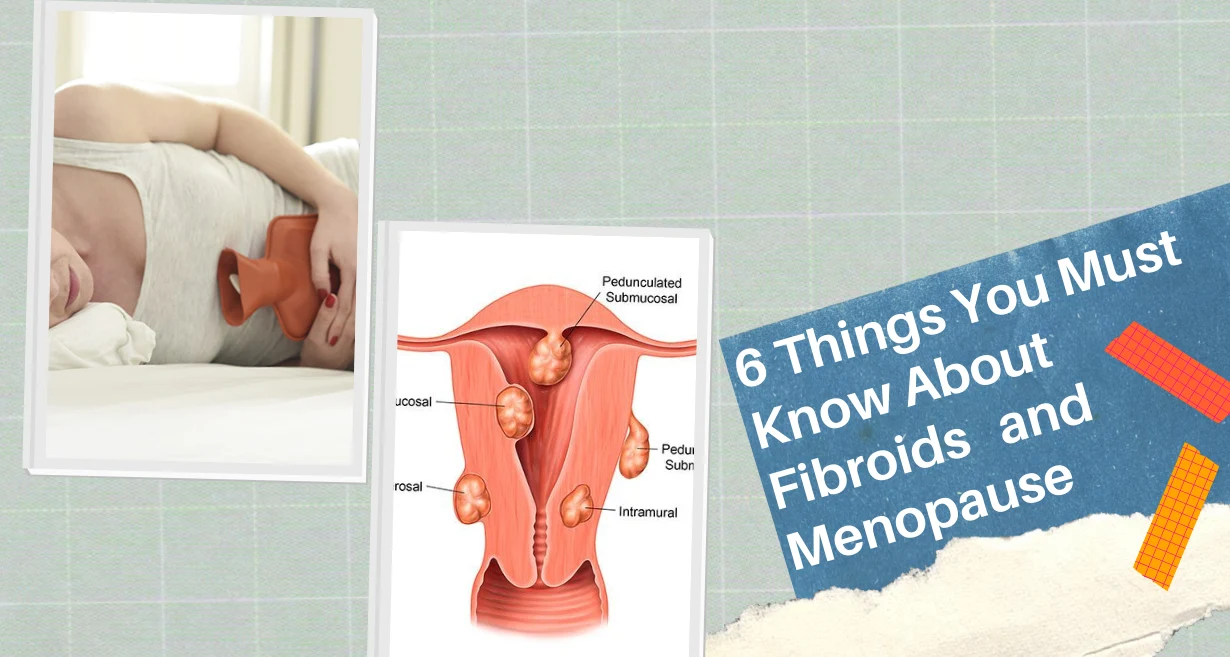
Calcified fibroids, also referred to as calcified leiomyoma, are non-cancerous growths that materialize in the muscular wall of the uterus. Over time, these fibroids can undergo a process of calcification, where calcium deposits accumulate within the fibrous tissues.
This calcification causes the fibroids to harden and become less responsive to hormonal changes, potentially leading to symptoms like pelvic pain, heavy menstrual bleeding, and discomfort.
While some calcified fibroids may not cause noticeable issues, others can result in complications and fertility problems. Understanding the nature and implications of calcified fibroids is crucial for women’s health management and treatment decisions.
Related Blog: 20 Dietary Changes to Reduce Fibroid Growth
Symptoms of Calcified Fibroids
Symptoms of calcified fibroids can vary in severity depending on the size, location, and number of fibroids present. Some women may experience no noticeable symptoms, while others may encounter significant discomfort and complications. Common symptoms of calcified uterus fibroids include:
- Heavy Menstrual Bleeding
One of the primary symptoms is excessive and prolonged menstrual bleeding, leading to the need for frequent pad or tampon changes and potential anemia.
- Pelvic Pain and Pressure
Calcified fibroids can cause pelvic pain or pressure, which may be dull or sharp and worsen during menstruation or sexual intercourse.
- Abdominal Enlargement
In some cases, larger fibroids can cause the abdomen to expand, giving the appearance of weight gain or pregnancy.
- Urinary Problems
Fibroids located near the bladder can lead to increased frequency of urination or difficulty emptying the bladder fully.
- Constipation
Fibroids situated near the rectum can exert pressure on the bowels, resulting in constipation or discomfort during bowel movements.
- Back Pain
Fibroids growing on the back of the uterus may cause back pain or discomfort.
- Infertility and Pregnancy Complications
Calcified fibroids can affect fertility by interfering with the implantation of a fertilized egg or obstructing the fallopian tubes. They may also increase the risk of miscarriages, preterm labor, or complications during pregnancy.
Causes of Calcified Fibroids
The exact cause of calcified fibroids is not completely comprehended, but several factors are believed to contribute to their development. Uterine fibroids, including calcified ones, are thought to arise from abnormal growth of smooth muscle cells in the uterine wall. The following factors are considered potential contributors to the formation of calcified fibroids:
- Hormonal Imbalance
Hormones, particularly estrogen and progesterone, play a significant role in the growth and maintenance of the uterine lining during the menstrual cycle. Hormonal imbalances, like excess estrogen, can stimulate the growth of fibroids.
- Genetic Predisposition
A family history of uterine fibroids can increase the likelihood of developing them. Specific genetic mutations may be associated with a higher risk of fibroid formation.
- Age and Hormonal Changes
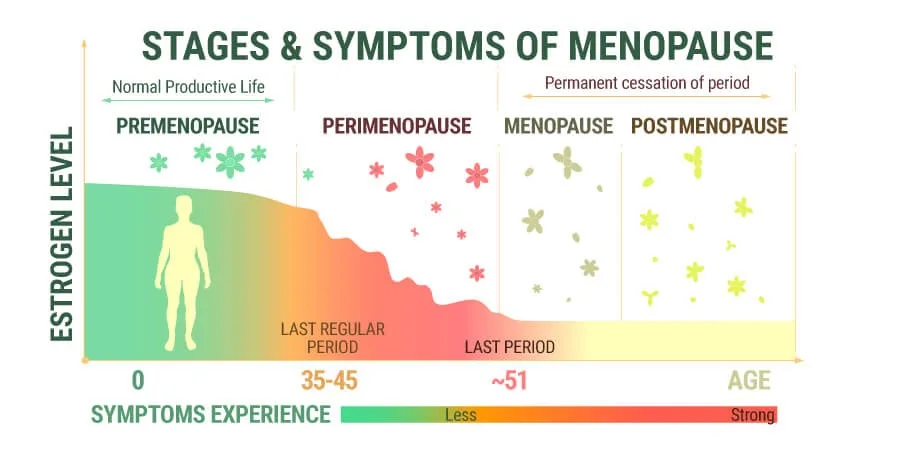
Calcified fibroids are more commonly diagnosed in women between the ages of 30 and 50. Hormonal fluctuations during this time, such as those experienced during pregnancy and perimenopause, can influence fibroid growth.
- Race and Ethnicity
Studies have shown that women of African descent are more susceptible to developing fibroids, including calcified fibroids, compared to women of other ethnic backgrounds.
- Obesity
Extra body weight has been tied to an increased risk of fibroid development, likely due to higher levels of circulating estrogen in obese individuals.
- Diet
A diet rich in red meat and deficient in fruits and vegetables may be linked with a higher risk of fibroids.
- Vascular Factors
Blood vessels play a role in the growth of fibroids, and abnormal vascular changes could contribute to calcification within the fibroids.
- Prior Uterine Trauma
In some cases, previous uterine trauma, such as surgeries or infections, may trigger the development of fibroids.
Related Blog: 6 Things You Must Know About Fibroids and Menopause
Calcified Fibroids Treatment Options
The treatment options for calcified fibroids depend on the severity of symptoms, the size and number of fibroids, and the woman’s overall health and reproductive plans. While some women may not require treatment if they are asymptomatic, others may seek relief from bothersome symptoms or fertility-related concerns. The primary treatment options for calcified fibroids include:
- Watchful Waiting
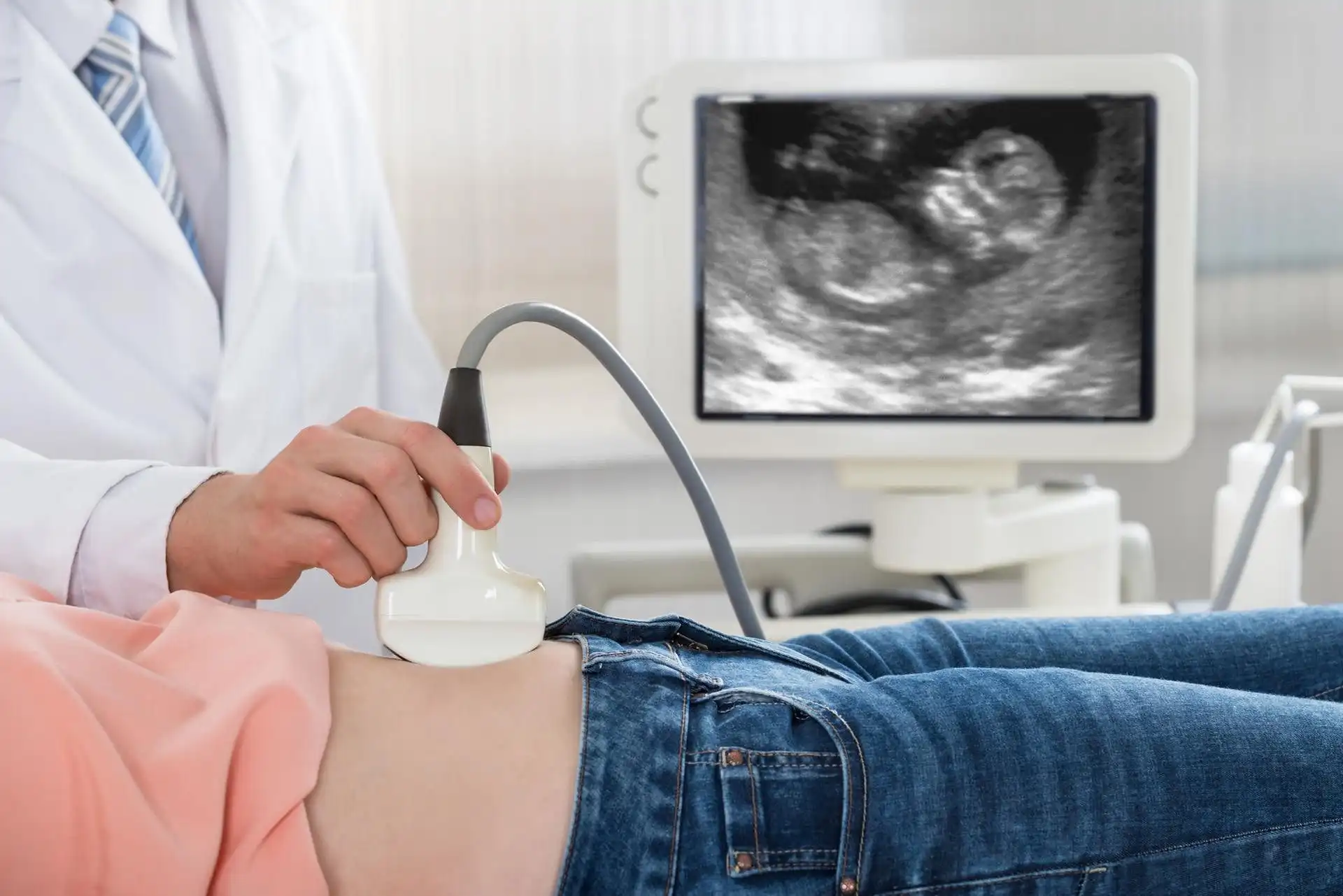
In cases where the fibroids are small, asymptomatic, or not affecting fertility, doctors may opt for watchful waiting. Regular monitoring through pelvic exams and ultrasounds is essential to track any changes in size or symptoms.
- Medications
Hormonal medications, such as gonadotropin-releasing hormone (GnRH) agonists, can be prescribed to temporarily shrink fibroids and alleviate symptoms. However, these medications are not a permanent solution, and symptoms may return after discontinuing treatment.
- Non-Invasive Procedures
Minimally intrusive procedures, like uterine artery embolization (UAE) or magnetic resonance-guided focused ultrasound surgery (MRgFUS), are options for fibroids that are causing significant symptoms. UAE involves blocking the blood supply to the fibroids, while MRgFUS uses focused ultrasound waves to destroy fibroid tissue.
- Myomectomy
Myomectomy is a surgical process that concerns removing fibroids while preserving the uterus. It is a suitable option for women who wish to retain their fertility or do not want to undergo a hysterectomy.
- Hysterectomy
Hysterectomy is the surgical expulsion of the uterus and is considered a definitive treatment for calcified fibroids. It is typically recommended for women who have completed their family planning or have severe symptoms that do not respond to other treatments.
- Endometrial Ablation
This procedure is used to treat heavy menstrual bleeding caused by fibroids. It involves destroying the uterine lining to reduce bleeding.
- Focused Ultrasound Surgery
This non-invasive procedure uses focused ultrasound waves to heat and destroy the fibroid tissue.
Conclusion
Calcified fibroids are non-cancerous growths that develop in the uterus and undergo calcification, potentially causing a range of symptoms like heavy bleeding, pelvic pain, and fertility issues. While the exact causes remain unclear, hormonal imbalances and genetic characteristics are believed to play a part. Treatment options vary from watchful waiting to surgical interventions, relying on the stringency of symptoms and individual preferences.
If you or someone you know is experiencing symptoms of calcified fibroids seek expert care at Queen’s Gynecology in Delhi. With our state-of-the-art facilities and skilled gynecologists, we provide accurate diagnoses and the best treatment plans.
FAQ’s
The decision to remove calcified uterine fibroids depends on the severity of symptoms and individual circumstances. Depending on case to case basis, some may require removal, while others may not.
The best treatment for calcified fibroids depends on the individual’s symptoms and preferences, ranging from watchful waiting to surgical interventions.
If you have calcified fibroids, it’s crucial to confer with a healthcare provider for appropriate evaluation and proper management.